Coping with Covid-19
This article was written early in the Covid pandemic. I think I did a pretty good job given how little information was available at the time. My current recommendations are simpler: Get vaccinated, and get on with your life. Don’t be afraid. Get Covid and move on. I think we’re all going to get it eventually, and living in fear is not the answer. You don’t need a mask except to protect others who are unable to get vaccinated yet. So wear your mask where required, and help protect those people. Check the CDC website for updates.
Coping with Covid-19: Information, and Suggestions for Appropriate Action
It has been my experience that fear of the unknown is the most powerful and debilitating of all fears.
Human beings, with our highly developed imaginations, create the most horrible outcomes in fantasy, and the fear of those outcomes can lead to unnecessary stress, panic, anger, and even paralysis.
The huge social impact of the current Covid-19 outbreak, with its orders to stay-at-home, quarantine, and social distancing, when combined with the current levels of distrust of government, misinformation spread on the internet, and even just a normal lack of understanding of non-medically-trained people all combine to create an atmosphere of fear and worry, and an environment where rumor and misinformation lead to unnecessary and counter-productive feelings and actions.
To counter and attempt to allay unnecessary fear, I am hoping this summary of facts, and my recommendations on appropriate actions and attitude will be helpful to you and those you care about. These are not “official” recommendations. See the CDC link below for those. Read, learn, and make up your own, informed mind.
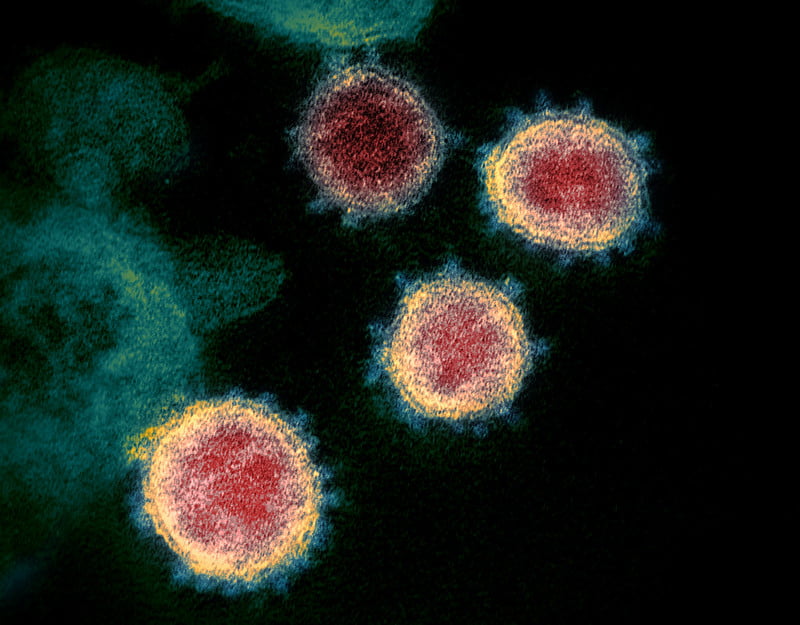
The Covid-19 virus is a coronavirus, a family name derived from their silhouette under x-ray microscopy, which resembles a ring or crown with jewels jutting out from it. Most coronaviruses infect non-human animals, but a few have evolved or changed structure in a way that allows them to infect humans. Covid-19 seems to have made this change in November 2019 in China, and it is rapidly spreading across the globe.
Coronavirus infections usually begin with respiratory symptoms, such as coughing, sneezing, or runny nose, and in bad cases cause pneumonia (lung infection) and difficulty breathing. They can also cause fever, aches and pains. Sometimes they cause diarrhea. Most coronavirus infections are mild: The common cold is caused by a coronavirus. But some coronaviruses have a tendency to cause severe illness: SARS and MERS are examples. Covid-19 does not seem to be as frequently lethal as SARS or MERS, but it infects more easily. For most people it causes a mild to moderate (think anywhere from common cold, to laid-out-at-home-in-bed for awhile) illness. However for some people, perhaps one in ten to one in twenty, it causes a severe illness requiring hospital support. Perhaps around 1%, or one in a hundred, could die from this infection, depending on the availability of appropriate hospital support.
Coronavirus spreads in multiple ways:
A common route is through minute droplets in the air which are sent there by infected people who sneeze without covering their mouths. These droplets are then inhaled by nearby people into the lungs or mucous membranes of the respiratory tract.
Another common way is through touching the hands of an infected person who has blown their nose, or blocked a sneeze into their hand and not washed their hands afterwards.
Another possibility is that the virus will be picked up from an object or surface that has been coughed on or touched by the unwashed hands of an ill person.
Once the virus has been transferred to your hands, unless you wash them, it is only a matter of time until you touch your mouth, your nose, or your eyes, the preferred access points to begin a new infection.
Covid-19 seems to be relatively hardy as coronaviruses go. It can remain infectious several hours floating in the air in enclosed spaces, or several days on hard metal or glass surfaces, before becoming deactivated or “killed”.
Armed with this information, we can better understand the situation, how we can best protect ourselves and our loved ones, and how to stay calm and informed.
First, given my estimate that the risk of serious illness leading to hospitalization is between one in ten to one in twenty, you as an individual likely do not need to fear infection. The odds are very much in your favor that you will have a mild or moderate illness, recover completely, and go on about your life. So stay calm.
The reason we are taking all these precautions, and making all these sacrifices, is to give the unlucky few the best possible chance of survival. Their lungs will become so infected they will temporarily need the help of machines to help them breathe. Unfortunately, viral infections can be very difficult to treat, and in severe cases of Covid-19 infection the best doctors can do is to help the person breathe until their immune system learns to fight the virus off on its own, and try to moderate a sometimes deadly over-the-top immune system response.
Even though one in twenty seems like a pretty small number, when we are talking about hundreds of thousands or millions of infected people, it is pretty clear hospitals will at some point be overwhelmed and the number of available breathing machines or “ventilators” will be used up. For that reason, authorities are attempting to slow down the rate of spread of the infection through the population. That way the ventilators and hospital beds used by those who get sick first can be re-used by those who get sick later, and more people will survive. This is what is meant by the buzz-phrase “flattening the curve“.
The development of a vaccine for this virus is moving at a very fast pace, yet any vaccine needs to be tested for safety and efficacy and that takes time. At least a year I would guess. Since the only “cure” for a viral infection is through vaccination, or by getting the infection and recovering, it is likely most of us will eventually get this infection. The optimal time for that to occur is later in the infection’s spread, when hospitals have the capacity to take care of us if we are one of the unlucky few who get seriously ill. Treatments also evolve, and doctors will find better and better treatments. Deadly viruses also tend to mutate to less deadly viruses as they spread through populations. Thus, 1 in 20 today may become 1 in 40 in a year or two.
Tests for Covid-19 come in two types: Antigen tests, and antibody tests. Antigen tests are useful for detecting active infections. They test for bits of actual virus that ill people shed in their throats. Antibody tests are useful for confirming that someone has had the illness after they are better. They detect that our immune system has created substances that bind to the virus and help to deactivate it.
Covid-19 will be with us long-term. Until a effective vaccination becomes available to the general population, we need to learn to live with it yet remain productive. The current “lock-down” situation is not sustainable over the long-term for many of us who need to work in order to survive. If we cannot pay our bills, eventually we will be homeless. A balance needs to be struck between caution and prevention, and being able to function so we can earn the money we need to survive. What follows are my thoughts about how to strike that balance, depending on your circumstances:
Case 1) You have already been exposed, gotten ill, and it is now two weeks since you have fully recovered.
Get tested for Covid-19 when you can. The best test would a combination of an antibody test to make sure your immune system has responded properly, along with an antigen test to prove the you are no longer infectious. There are reports that some people recover, but still shed virus. This dual-test protocol would show an individual was both safe from being infected again, and not a threat to others who have not yet been infected. If there is a scarcity of testing available, follow Case 2 recommendations below until you can be tested.
Congratulations! You are free to do as you wish. You do not need to wear a mask or gloves, or be concerned about infecting others. Get back to work and enjoy your life as before!
Case 2) You have not been exposed, as far as you know, and are otherwise healthy.
This is the situation most of us are currently in I would guess. Here is a balanced approach I recommend:
For now, maintain social distancing as much as possible. At some point we will have to let that go, so read Case 5 below. When in enclosed places like supermarkets, stores, subway cars, trains, or buses, wear a face mask or cover your mouth and nose with a scarf or cloth. While an approved, certified, and well-fitting N95 face mask is best, until they are more widely available, using some sort of face and nose covering will help. I read one study which said these face coverings were “only” 89% effective. Not enough if you are working in a hospital or clinic, but very helpful if you only have an occasional exposure. Gloves are optional. Mostly they remind for us not to touch our face with our hands. Frequent hand-washing with soap and water when we come home from being outside, or after shaking hands or touching hard surfaces in enclosed spaces outside your home is what I practice. Using an alcohol-based hand sanitizer can be a useful supplement when hand-washing is not possible. Goggles are optional, unless you are working in a hospital or are in frequent contact with infected people. I wear glasses, so I have some protection from an inadvertent sneeze, and having them on makes me more aware when I reach up with my hand to rub my eyes (Don’t, unless you are at home and sure your hands and face are clean). Consider wearing sunglasses or getting some non-prescription glasses to wear when you are out and about. If you are outside and it is not crowded, like in a park, feel free to take off your mask. Go for a run, be active. Certain sports, like tennis, should be fine if played outdoors and social distancing is maintained. If you are a family, you can go to the park together, play ball, and run around as you wish. Maintain social distancing with non-family members. Kids can be forgetful, but be a good role model for them, stay calm, and make sure everyone washes up well when they get home. Hands first, then the face.
Case 3) You are currently feeling OK, but you have an underlying health issue (asthma, lung disease, immune compromise, diabetes or old age) which makes you at high-risk for developing severe illness should you become infected.
Follow Case 2 and Case 6 recommendations at a minimum. If you go out, wear a well-fitting N95 mask, gloves, and goggles if at all possible. When you return home, wash your hands well, then your face. If you are coughed on while you are out, take off your clothes when you come in and put them in the washing machine. Then wash your hands and goggles and put your re-usable face mask in the washer as well. Then wash your hands again, and then your face. Carry on.
Case 4) You are feeling ill, and worry you might have gotten Covid-19.
Stay home, and quarantine yourself as much as possible. Unless you have difficulty breathing, you probably don’t have to go to the hospital, but check with your doctor. If an antigen-based test is readily available where you live, you could get that done to verify you actually have Covid-19 and not some other infection. If not, just assume you are infected for now. Rest, and drink plenty of fluids. Allow yourself to have a moderate fever. Fever is a natural response to infection, and helps your body be more effective fighting off germs. If your fever is extreme, or aches and pains are too much, there are reports acetaminophen may be safer to use than ibuprofen for this infection. If you must go out – say to get food or go to the doctor’s office, wear a face mask or face covering, and wear some gloves if at all possible. Use hand-sanitizer and wash your hands frequently. Try to minimize touching things others may touch. If you cough or sneeze, make sure you cover your mouth with your elbow, or into a tissue. If you have visitors, make sure to warn them you are ill. You should all wear masks or face coverings. Crack the windows to let fresh air circulate while they are there. They should wear gloves and also goggles or glasses. Remind them to take off their gloves when they leave, and when they get home, to wash their hands first, and then their face well. When you are feeling better, see Case 1!
Case 5) You are caring for a family member who may be ill with Covid-19.
Follow the recommendations in Case 4. If you can, isolate your ill family member to a separate room. Consider opening the window once in awhile in the room to let fresh air circulate, but keep the room temperature comfortable. When you are in the room, wear a mask, or cover your face, nose and eyes as best you can. Keep your patient warm and comfortable, but let them have a mild to moderate fever. Wash your hands, and then your face after you leave the room. Change your towels frequently. If your ill family member is older and doesn’t mind, they can wear a mask. If it is a child, I don’t recommend a face mask because they make breathing more difficult and children’s diaphragms are not as strong as an adults. Though children don’t seem to get seriously ill as frequently as adults from this infection, it does happen. If they become lethargic, stop drinking, or have difficulty breathing, get in touch with their pediatrician or go to the emergency room.
Recommendations For The New Normal:
Case 6) You are otherwise healthy, have not been yet been infected, but you need to be in an environment where you are in close proximity to others who may or may not be infectious.
Once the current, unsustainable, stay-at-home restrictions are lifted; as they must be if we are to survive long-term as a society, this will likely become the new normal. We have to get back to work.
The protocols have not yet been agreed on, but here are my suggestions:
Generally, follow the recommendations I laid out in Case 2. Unless your job is outside, wear a re-usable or disposable face mask and glasses or goggles at work. Wear gloves, or wash your hands after handling possibly contaminated objects or surfaces.
If you work in an office, wipe down your keyboard, handles and desk in the morning, and you won’t need gloves.
If you are a truck driver, make sure you wipe down handles, steering wheels, and gear shift levers before starting off. Use gloves when loading and unloading cargo, or be sure to use a hand sanitizer frequently.
Hospital workers need to follow hospital protocols. The above is a minimum for them.
At some point, I don’t see why we can’t get back to our usual social activities. We could play poker with friends, watch movies, have block parties and picnics, and go to the ball game with proper protection such as a re-usable face mask, glasses or goggles, and hand wipes, sanitizing lotion, or gloves. Wash your hands before and after using a public rest room, and after drinking from a public water fountain. If you are dating, I recommend that for the first two weeks, when you meet in person you use full precautions with no physical contact. Hopefully if both of you are following these recommendations it will be safe to have personal contact after that. If one of you gets exposed to someone who is ill, you should start the two week precaution period again. The same is true if a family member has an exposure. However, children need hugs and the reassurance of touch. Just wear gloves, or wash your hands afterwards. Again, small children should not wear face masks. We will need to develop a protocol for those who have already been infected and are no longer infectious as in Case 1. Perhaps a card could be worn or carried, signed by a doctor or health official, so these people would not need to wear protective gear at work if they didn’t want to.
I hope this information, and these suggestions are helpful to you and those you love. Lets go about our lives productively and with enjoyment, despite Covid-19. With appropriate caution, but a minimum amount of fear. Armed with knowledge, and with some simple precautions, Covid-19 need not destroy our society or our mental health!
Best wishes and good luck to all!
P.S. Think about my recommendations, and about getting back to normal. Does this make sense to you? Do you have other suggestions? I plan on updating this page in light of your comments and as current knowledge evolves. Check back for updates periodically. If you have a question or comment, please leave it below! You never know who might benefit from it!
Links to online resources:
How to make a re-usable face mask.
How to make hand sanitizer.
Free online group meeting to share concerns and solutions with others.
Centers for Disease Control and Prevention Covid-19 Site
Originally Published March 29, 2020

0 Comments